Sermorelin is a synthetic analog of growth hormone–releasing hormone (GHRH). It stimulates the pituitary to release endogenous growth hormone, which may increase downstream IGF-1 levels. It was historically FDA-approved for pediatric GH deficiency but is commonly discussed in research contexts for adult GH support.
Typical research descriptions emphasize:
 Mimicking natural physiology by stimulating GH release rather than replacing GH directly
Mimicking natural physiology by stimulating GH release rather than replacing GH directly
 Once-daily subcutaneous administration
Once-daily subcutaneous administration
 Bedtime dosing to align with natural nocturnal GH pulses (peak secretion occurs during sleep)
Bedtime dosing to align with natural nocturnal GH pulses (peak secretion occurs during sleep)
Important context:
•Many products marketed today are labeled research use only and are not FDA-approved medications.
•Protocols vary widely in research literature.
⸻
Reconstitution (educational reference)
Given:
•Vial: 10 mg Sermorelin (lyophilized powder)
•Diluent: 2.0 mL bacteriostatic water (BAC water)
•Syringe: U-100 insulin syringe (100 units = 1 mL)
Step overview (general sterile research handling)
1.Add 2.0 mL BAC water slowly into the vial.
2.Aim the stream against the vial wall to reduce foaming.
3.Gently swirl — do NOT shake vigorously.
4.Allow ~15–20 minutes for full dissolution.
⸻
Resulting concentration (key math)
Total drug = 10 mg
Total volume = 2 mL
 Concentration:
Concentration:
 5 mg/mL
5 mg/mL
or
 5000 mcg/mL
5000 mcg/mL
⸻
U-100 syringe conversion
A U-100 insulin syringe:
•100 units = 1 mL
•1 unit = 0.01 mL
Now convert:
 5000 mcg per 1 mL
5000 mcg per 1 mL
 50 mcg per 1 unit
50 mcg per 1 unit
Simple rule for this specific mixture:
1 unit on the syringe = 50 mcg Sermorelin
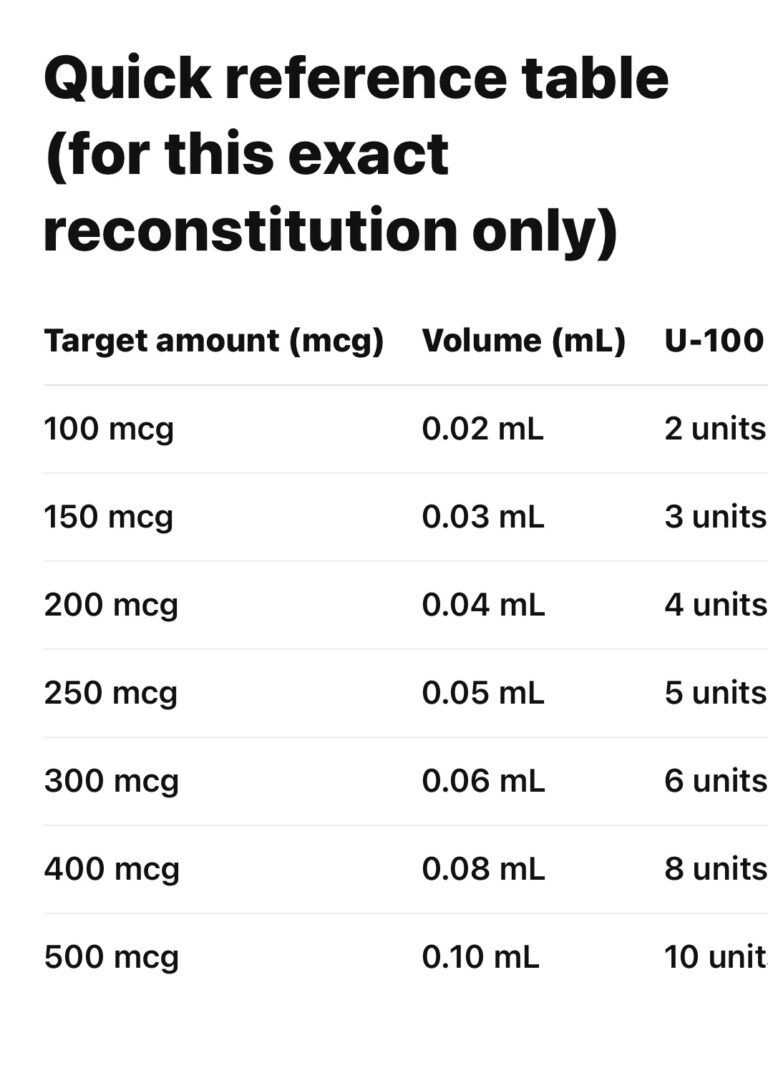
Published protocols and clinic literature commonly describe:
•Range often discussed: 100–300 mcg once daily
•Administration: subcutaneous injection
•Timing: bedtime to align with natural GH pulsatility during sleep
Again, this varies depending on study design or practitioner methodology.
⸻
Additional research notes
•Store reconstituted peptide refrigerated (commonly 2–8 °C).
•Avoid repeated agitation.
•Use sterile technique for each withdrawal.
•Potency duration after reconstitution varies by manufacturer and handling.